What are the odds of getting Lyme disease from a tick?

Finding a tick attached to your skin is a jarring experience, but it is rarely an emergency that necessitates immediate panic. The initial reaction is often fear of developing Lyme disease, yet statistics suggest that the probability of transmission from a single tick bite is significantly lower than most people assume. While Lyme disease is the most common vector-borne illness in the United States, the majority of ticks, even in endemic areas, do not carry the bacteria Borrelia burgdorferi. [2] Understanding the specific factors that govern transmission can help replace anxiety with clear, actionable logic.
# Infection Odds
When you find a tick, your mind might jump to the worst-case scenario, but the math is generally in your favor. Even in regions where the disease is widespread, the risk of acquiring Lyme disease from a single bite is typically estimated at less than 3%. [1][10] This percentage fluctuates based on where you live and the species of tick involved. For example, in highly endemic areas, the likelihood might be slightly higher, while in low-risk zones, it remains statistically negligible. [6][10]
It is important to remember that a bite does not equate to infection. The tick must be infected, it must bite you, and it must remain attached for a sufficient duration to facilitate the transfer of the bacteria. [1] Because the tick must first ingest a blood meal and then transmit the pathogen, the timeline is your greatest ally. [4] Finding a tick early and removing it correctly changes the equation entirely, often dropping the transmission risk to nearly zero. [5]
# Transmission Mechanics
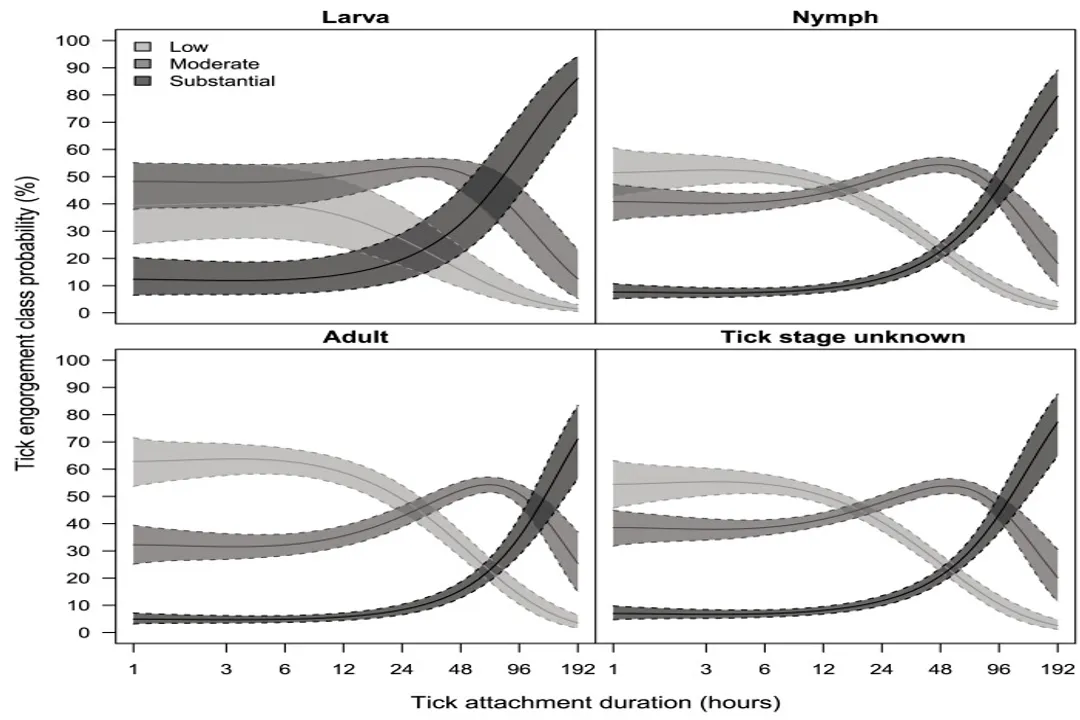
Transmission is not instantaneous. Unlike a mosquito, which can transmit diseases almost immediately upon biting, ticks require a prolonged feeding period. [4] The bacteria causing Lyme disease reside in the tick’s midgut. Before they can enter the host’s bloodstream, they must travel to the salivary glands, a process that typically requires the tick to be engorged with blood. [2]
Research indicates that this transition generally requires the tick to be attached for at least 36 to 48 hours. [1][4] If you remove the tick within the first 24 hours, the chances of contracting Lyme disease are exceedingly low because the bacteria have likely not had sufficient time to migrate and infect the host. [4] This biological delay is the primary reason why daily tick checks are the most effective method for preventing disease. [9]
# Geographic Context

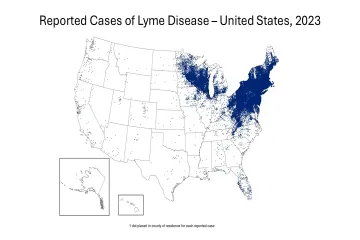
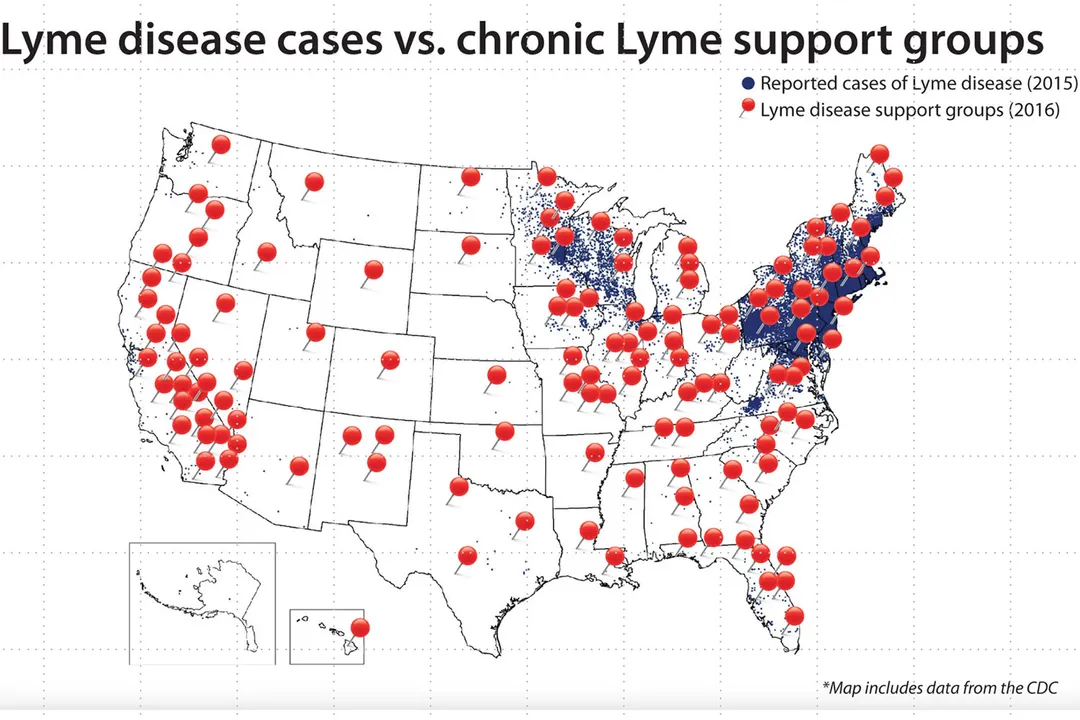
Geography acts as a primary filter for risk. Lyme disease is not distributed uniformly; it is heavily concentrated in specific regions, primarily the Northeast, the mid-Atlantic, and the North-Central United States. [2][6] Within these regions, the black-legged tick, or Ixodes scapularis, is the primary carrier. [2] If you are in an area where this species is not prevalent, the probability of contracting Lyme disease from a random tick bite effectively plummets. [1][6]
Even within endemic states, tick infection rates vary wildly by county and even by local habitat. A tick caught in a dense, brushy forest in a high-risk state has a different risk profile than one found in a manicured lawn or a different climate entirely. [6] Contextualizing the bite based on your location and environment is a crucial step in assessing the actual danger level, rather than defaulting to universal panic. [1]
# Lifecycle Stages
The age of the tick plays a substantial role in its ability to transmit disease. Ticks have four life stages: egg, larva, nymph, and adult. [2] Nymphs are the stage most responsible for human infection. [4] These ticks are roughly the size of a poppy seed, making them exceptionally difficult to spot. [1] Because they are so small, they often go unnoticed on the body, allowing them to remain attached long enough to transmit the bacteria. [4]
Adult ticks are larger and easier to see, which means they are usually discovered and removed much faster than nymphs. [1] While an adult tick is more than capable of transmitting the disease, its size makes it a more visible target during a routine body check. [4] The "nymph window," typically occurring in late spring and early summer, is the peak period for human infection not necessarily because the nymphs are more aggressive, but because they are more elusive. [1][4]
# Proper Removal
When you discover an attached tick, the method of removal is vital. Many myths exist about using nail polish, petroleum jelly, or heat to force the tick to detach. These methods are ineffective and can potentially cause the tick to regurgitate its stomach contents into the wound, which increases the risk of infection. [2][4]
The correct approach is simple and mechanical:
- Use clean, fine-tipped tweezers.
- Grasp the tick as close to the skin surface as possible—aiming for the head, not the body.
- Pull upward with steady, even pressure.
- Do not twist or jerk the tick, as this can break the mouthparts off and leave them in the skin. [4]
After removal, clean the bite area and your hands with rubbing alcohol or soap and water. [4][9] If the mouthparts remain in the skin, you can try to remove them with tweezers, but if they are difficult to extract, it is best to leave them alone and let the skin heal, as they are not the source of the bacteria. [4]
# Symptom Monitoring
Removal is only half the process; the next phase is observation. For the first few weeks after a tick bite, monitor the site and your overall health. Many people worry about the "bullseye" rash, or erythema migrans, which is a hallmark sign of early Lyme disease. [7] This rash can appear as a red circle with a clearing in the center, though it does not always present in this classic pattern. [9]
Beyond the skin, keep an eye out for flu-like symptoms. These include fever, chills, fatigue, body aches, joint pain, and swollen lymph nodes. [7] If these symptoms appear, seek medical attention immediately. Early treatment with antibiotics is highly effective and significantly prevents the development of more serious long-term complications. [2][9] Not everyone who contracts Lyme will show a rash; therefore, unexplained illnesses during peak tick season should always be evaluated by a healthcare professional with the context of the recent bite. [9]
# Risk Profiles
To better understand the variance in risk, consider the following matrix. This helps differentiate between a "low-concern" bite and one that warrants a doctor's visit.
| Factor | Lower Risk | Higher Risk |
|---|---|---|
| Attachment Time | < 24 hours | > 36-48 hours |
| Tick Size | Adult (visible) | Nymph (poppy seed size) |
| Geography | Low-prevalence zone | Endemic hotspot |
| Removal Method | Proper (tweezers/steady pull) | Improper (heat/burning/twisting) |
| Symptoms | None | Rash, Fever, Aches |
Note: This table serves as a conceptual guide for risk assessment. Regardless of the profile, persistent symptoms should always be evaluated by a medical professional.
# Actionable Strategy
When you are out in nature, the best defense is a proactive routine. Creating a "tick protocol" can significantly reduce your encounters. When returning from hiking or gardening in potentially tick-heavy areas, place your clothes in the dryer on high heat for 10 minutes; this is often more effective at killing ticks than washing alone, as ticks are susceptible to the dehydration caused by dry heat. Showering within two hours of coming indoors also allows you to wash off unattached ticks and perform a thorough full-body inspection. [9]
It is also helpful to keep a record. If you find a tick, take a photo of it before you dispose of it. If you develop symptoms later, having a clear image of the tick—or the bite site—can help your doctor make a more informed diagnosis. [7] Some people choose to save the tick in a small container or baggie for testing, but many public health departments advise against this, noting that laboratory testing of ticks is often inaccurate and not a reliable guide for clinical decision-making. [2] Prioritizing your own symptom monitoring over testing the tick is generally the more effective clinical strategy.
The psychological weight of a tick bite is often heavier than the physical risk. By shifting focus from the fear of the encounter to the mechanics of prevention and early detection, you can safely navigate outdoor activities. Most bites do not result in illness, and for those that do, medical intervention is highly effective when sought early. Keep the area clean, watch for warning signs, and rely on the biological reality that transmission requires time, which you largely control through vigilance.
Related Questions
#Citations
Ticks And Lyme Disease: 3 Factors Determine Risk Of Infection - NPR
How Lyme Disease Spreads - CDC
Predicting the risk of Lyme borreliosis after a tick bite, using a ... - PMC
Ticks and Lyme Disease | Johns Hopkins Medicine
Tick Bite? Don't Panic - UConn Today - University of Connecticut
Lyme Disease - Illinois Department of Public Health
Keep a Lookout for Symptoms from Tick Bite This Summer
What are the odds of if you get bit by a tick that you get lyme disease ...
American Lyme Disease Foundation
Professor Hovius: this is how much chance you have of contracting ...