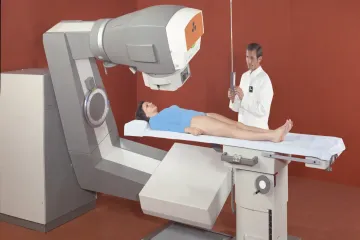
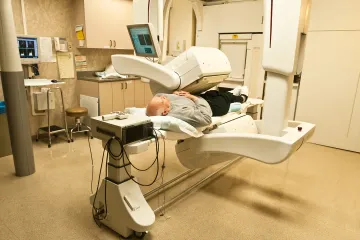
What is radiation therapy for prostate cancer?

Radiation therapy stands as a primary medical option for treating prostate cancer. It functions by using high-energy beams or implanted radioactive material to damage the DNA within cancer cells. [1][2] When this DNA becomes damaged, the cancer cells stop dividing and eventually die, allowing the body to break them down and eliminate them. [5] Because the prostate is a small organ, radiation can be directed with high precision to kill tumor cells while sparing much of the healthy tissue in the surrounding area. [3][6]
Deciding on this treatment depends on factors such as the stage of the cancer, the patient’s overall health, and personal goals regarding side effects and recovery time. [2][9] Many patients choose radiation because it is a non-surgical option that can effectively control or eliminate localized cancer. [6][8]
# External Radiation
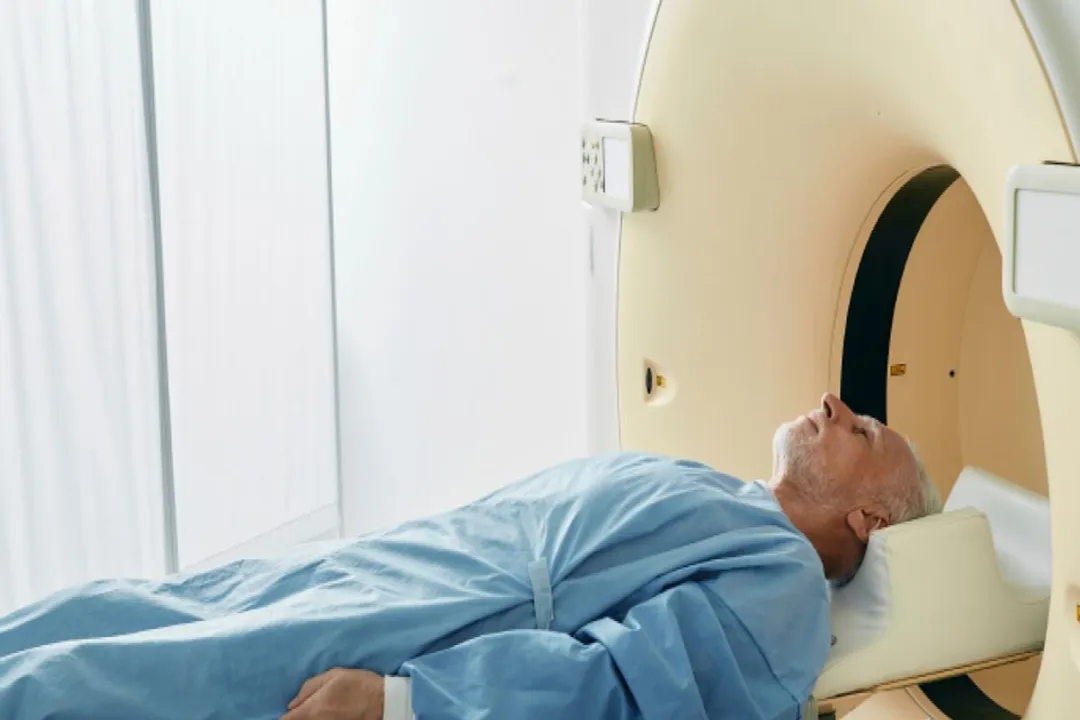
External beam radiation therapy (EBRT) is the most common form of this treatment. [2] During this process, a machine moves around the body, aiming beams of energy directly at the prostate. [1] The patient lies on a table, and the machine does not touch the skin, making the session similar to receiving an X-ray, though the energy levels are significantly higher. [10]
Several modern techniques have refined how this energy is delivered:
- Intensity-Modulated Radiation Therapy (IMRT): This method uses computer-controlled beams to sculpt the radiation dose to the exact shape of the prostate. [2][6] By modulating the intensity of the beams, doctors can deliver higher doses to the tumor while minimizing exposure to the bladder and rectum. [8]
- Image-Guided Radiation Therapy (IGRT): This involves taking daily images of the prostate immediately before or during treatment sessions. [2] Because the prostate can move slightly depending on how full the bladder or rectum is, IGRT allows the medical team to adjust the beam placement in real time to maintain accuracy. [6]
- Stereotactic Body Radiation Therapy (SBRT): Often called SBRT or stereotactic ablative radiotherapy, this technique delivers very high doses of radiation over a shorter timeframe, typically five sessions or fewer, compared to the standard course that might last several weeks. [2][8]
Proton therapy is another specialized form of external radiation. [4] Unlike standard X-ray (photon) beams that pass through the body, protons can be calibrated to stop once they reach the tumor. [4][5] This potentially reduces the radiation dose that affects healthy tissues located behind the prostate, such as the rectum. [4]
# Internal Radiation

Internal radiation, also known as brachytherapy, involves placing radioactive material directly inside or very close to the prostate gland. [1][2] This approach allows for a very high dose of radiation to be delivered to a small area while quickly decreasing the dose just millimeters away. [3]
There are two main types of brachytherapy:
- Permanent Brachytherapy (Low-Dose Rate): Doctors use needles to insert small, radioactive "seeds" about the size of a grain of rice into the prostate. [1] These seeds are left in place permanently. They slowly release radiation over several weeks or months and then become inactive. [2] Because the radiation is contained, patients can usually return to normal activities fairly quickly. [3]
- Temporary Brachytherapy (High-Dose Rate): This method involves inserting hollow needles or catheters into the prostate through which radioactive sources are passed for a short amount of time—often only a few minutes—before being removed. [2] A patient might undergo a few treatment sessions over a day or two. [5]
# Treatment Process
The path to starting radiation therapy involves several steps to ensure accuracy and patient comfort.
- Consultation: A radiation oncologist reviews the patient’s medical history and PSA levels to determine if radiation is appropriate. [1]
- Simulation: Before treatment begins, the patient undergoes a planning session. This usually involves a CT scan or MRI to map the exact location, size, and shape of the prostate. [2][6] Small marks or tattoos might be placed on the skin to help align the equipment precisely for every session. [7]
- Treatment Planning: Medical physicists and dosimetrists work with the oncologist to calculate the exact angles and intensity of the beams. [6]
- Delivery: For external beam treatments, patients typically visit the center daily, five days a week, for several weeks. [2] Each session is short, often lasting only 15 to 30 minutes, with the radiation exposure itself taking just a few minutes. [6][8]
# Comparison Matrix
Choosing between external and internal options involves weighing specific variables. The following table provides a quick reference to distinguish these modalities based on typical clinical standards.
| Feature | External Beam (EBRT) | Permanent Brachytherapy | High-Dose Rate (HDR) |
|---|---|---|---|
| Duration | Weeks (e.g., 5-9 weeks) | Single procedure | 1-3 sessions |
| Invasiveness | Non-invasive | Minimally invasive (needles) | Minimally invasive (catheters) |
| Radioactive | No (leaves body instantly) | Yes (seeds remain) | No (source removed) |
| Typical Target | Localized/High-risk | Low-to-Intermediate risk | Intermediate/High-risk |
| Recovery | Immediate | Few days of discomfort | Few days of rest |
This table illustrates that while external beam therapy requires a longer time commitment for daily visits, it avoids the surgical placement of implants. [1][2] Conversely, brachytherapy offers a more concentrated dose but requires a minor procedural intervention. [3][5]
# Managing Side Effects
Radiation can affect surrounding organs, which may lead to specific side effects. These reactions are typically categorized into urinary, bowel, and sexual issues. [1][9]
- Urinary Symptoms: Patients may notice increased frequency, urgency, or a burning sensation during urination. [2] These symptoms often occur because the bladder is located next to the prostate and receives some incidental radiation. [6]
- Bowel Symptoms: The rectum is also close to the prostate. Radiation may cause inflammation, leading to loose stools, increased bowel movements, or rectal discomfort. [2][9]
- Sexual Function: Radiation can damage the nerves and blood vessels involved in erections. While side effects may not appear immediately, some patients notice a gradual decline in erectile function over time. [1][5]
Medical teams often prescribe medications to manage inflammation and bladder spasms. [8] Furthermore, many patients find relief by adjusting their diet—avoiding caffeine, spicy foods, or alcohol can often help mitigate irritation in the bladder and bowel. [9]
# Optimizing Recovery
To ensure the best possible experience and manage the impact of treatment, patients can take proactive steps. While these suggestions are not substitutes for medical advice, they are standard practices recommended to assist during the treatment period.
- Bladder Protocol: Many centers require a full bladder for daily external treatments to move the bladder away from the prostate. Following the specific water-drinking schedule provided by the clinic is vital for consistent targeting. [6]
- Pelvic Floor Training: Starting Kegel exercises before radiation begins can strengthen the muscles that control bladder function. [9] This can improve recovery from urinary side effects after treatment concludes.
- Skin Care: During external radiation, the skin in the pelvic area can become sensitive. Using mild, fragrance-free soaps and avoiding tight clothing can prevent irritation in the treatment area. [10]
- Fiber Intake: To minimize bowel irritation, maintaining regular, soft bowel movements is key. Increasing fiber intake or using gentle stool softeners can prevent constipation and reduce pressure on the pelvic region. [9]
# Multidisciplinary Approach
Radiation therapy is rarely a solitary event. It is usually coordinated by a team that includes a radiation oncologist, who designs the treatment plan, and a medical physicist, who ensures the radiation is delivered safely. [6] Patients are encouraged to discuss the full spectrum of their health with this team, including their current medications and other existing conditions like diabetes or previous surgeries. [5]
Because prostate cancer management can involve multiple specialists—such as urologists, medical oncologists, and radiation oncologists—communication between these providers ensures that the treatment aligns with the overall disease strategy. [1][5] For instance, a doctor might combine radiation with a short course of hormone therapy to make the cancer cells more sensitive to the radiation beams, particularly in intermediate or high-risk cases. [2][8]
Understanding the specific mechanics of one's own treatment plan helps patients feel more prepared. Whether the treatment involves external beams or internal seeds, the goal remains consistent: to provide effective cancer control while preserving quality of life. Ongoing follow-up appointments after the completion of therapy are necessary to monitor PSA levels, which serve as a primary indicator of how well the treatment is working. [6][10]
#Videos
Radiation therapy for prostate cancer: What to expect - YouTube
Related Questions
#Citations
Radiation therapy for prostate cancer - Mayo Clinic
Side Effects of Radiation Therapy for Prostate Cancer
Radiation Therapy | Prostate Cancer Foundation
Navigating radiation therapy: a prostate cancer treatment guide
Radiation Therapy for Prostate Cancer
Radiation Therapy for Prostate Cancer | Johns Hopkins Medicine
Radiation therapy for prostate cancer: What to expect - YouTube
Radiation Therapy for Prostate Cancer
Radiation | ZERO Prostate Cancer
Radiation Treatment for Prostate Cancer - Buffalo, NY