How can diseases be treated?
Treating diseases is a complex, ever-evolving field that spans everything from immediate relief for acute infections to long-term strategies aimed at total prevention through global elimination. The approach taken depends entirely on what is causing the illness—be it a microscopic invader like bacteria or a virus, or perhaps an internal malfunction the body cannot correct on its own. For the general reader, understanding how medical science confronts illness requires looking beyond the single pill or shot, examining the diverse arsenal of tools available, from specific pharmaceuticals to supportive lifestyle changes that bolster our natural defenses.
# Disease Types

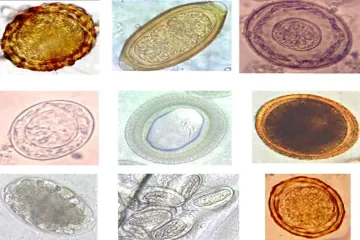
Infectious diseases, which arise from invading pathogens such as bacteria, viruses, fungi, or parasites, represent a major area of focus for treatment strategies. These pathogens can spread from person to person, animal to person, or through contaminated food, water, or surfaces. While infectious agents receive significant attention due to their potential for rapid spread, it is worth noting that many conditions causing high global mortality—some resulting in millions of deaths—are, in fact, treatable. Successful management, therefore, is not just about fighting off the flu but also ensuring access to effective therapies for chronic or common life-shortening conditions.
# Medical Attack
When a specific infectious agent is identified as the culprit, treatment often centers on targeted medical intervention designed to eliminate the pathogen or inhibit its ability to multiply within the host. The class of medication selected depends directly on the type of germ causing the trouble.
For bacterial infections, the cornerstone of treatment has long been antibiotics. These drugs work by killing bacteria or stopping their growth. However, the effectiveness of antibiotics is not guaranteed; the emergence of antibiotic-resistant bacteria means that a course of treatment that might have worked a decade ago may now be ineffective, requiring physicians to carefully select the correct drug and dosage to combat evolving microbial threats.
When viruses are involved, the treatment approach shifts. Antiviral medications are designed to interfere with the viral life cycle, preventing the virus from replicating inside human cells. Unlike antibiotics, which can often broadly target many types of bacteria, antivirals are typically highly specific to a particular virus or group of viruses. For example, specific antivirals are used to manage conditions like HIV or influenza.
Fungal infections, which are generally less common but can be serious, are countered with antifungal drugs that target the unique structures of fungal cells. Parasitic infections, such as malaria, require specialized antiparasitic medications to eliminate the parasite dwelling within the body.
The successful application of these antimicrobial therapies relies heavily on accurate diagnosis. Without precisely identifying the causative agent, treatment can be misguided, potentially wasting time or, worse, contributing to resistance if a broad-spectrum agent is used unnecessarily.
# Supportive Care
Treatment is rarely just about applying a weapon against the invader; it also involves supporting the patient's body as it fights back. This supportive care is critical, particularly when the disease itself—or the battle against it—causes significant distress or dysfunction.
Symptom management forms a large part of recovery. This can include using medications to control fever, alleviate pain, or manage symptoms like vomiting or diarrhea. In more severe cases, supportive care might involve hospitalization for intravenous (IV) fluids to prevent dehydration, or providing oxygen if breathing is compromised. The goal here is to maintain the patient’s physiological stability, allowing their own immune response and any prescribed medication the best chance to succeed.
When considering the entire treatment panorama for infectious diseases, a crucial distinction emerges between eradicating the pathogen from the body (the job of the drug) and preventing the host from succumbing to the illness (the job of supportive care). This is why a structured approach, often developed by infectious disease specialists, is necessary to coordinate these different efforts.
# Immunity Enhancement
While direct medication attacks the disease, an equally important, though often slower-acting, treatment strategy involves fortifying the body's internal defense mechanisms: the immune system. A well-functioning immune system can prevent infection entirely or rapidly clear a mild infection before it escalates. Enhancing immunity, therefore, acts as a proactive treatment measure against future threats and a supportive measure during current battles.
Several consistent lifestyle factors emerge across expert recommendations as foundational to immune health:
- Nutrition: Consuming a diet rich in vitamins and minerals is essential. Certain nutrients are necessary for the production and function of immune cells. Prioritizing fruits, vegetables, and lean proteins provides the building blocks needed for defense.
- Sleep Quality: Adequate, high-quality sleep allows the body to produce protective cytokines, which are small proteins important for fighting inflammation and infection. Chronic sleep deprivation impairs immune response.
- Physical Activity: Regular moderate exercise can improve the circulation of immune cells, allowing them to patrol the body more effectively. Over-exercising, however, can temporarily suppress immunity, highlighting that balance is key.
- Stress Management: High or chronic stress floods the body with hormones like cortisol, which can suppress the effectiveness of the immune system over time. Finding constructive ways to manage daily pressures is a direct intervention against disease vulnerability.
- Healthy Weight: Maintaining a healthy weight is linked to better immune function. Excess body fat can promote chronic, low-grade inflammation, which diverts immune resources and potentially exhausts the system.
It is important to recognize that while these lifestyle adjustments support overall health, they are not typically curative for an established, severe infection; rather, they optimize the environment in which drug treatments must operate. If we map this conceptually, the medical intervention (like an antibiotic) is the surgical strike, while immune enhancement is the logistical support ensuring the soldiers (immune cells) are well-fed and rested for the long haul.
# Eradication Aims
The most definitive form of disease treatment is not cure but eradication: the complete and permanent reduction to zero of the worldwide incidence of infection caused by a specific agent. This is a global public health intervention, far surpassing the scope of individual patient care.
Eradication is an exceptionally high bar to clear, as demonstrated by the success achieved with smallpox, a virus eradicated in 1980. Successful eradication programs typically require a combination of highly effective intervention tools, such as widespread vaccination, and a pathogen that cannot hide indefinitely in animal reservoirs or persist silently in the environment.
Diseases like polio are extremely close to this ultimate goal, having seen dramatic reductions thanks to decades of concerted global effort. Eradication, in essence, transforms a disease from a therapeutic problem requiring constant treatment and management into a historical footnote. It shifts resources away from reactive care towards other pressing health concerns.
If we consider the entire spectrum of treating disease, eradication represents the final, successful conclusion of a treatment program initiated decades earlier through preventative measures like mass immunization.
# Synthesis of Strategy
The treatment of disease is thus a layered defense. On the micro-level, treating an acute illness in a single patient involves swift diagnosis followed by targeted pharmaceutical attack (antibiotics, antivirals) coupled with meticulous supportive care to manage symptoms and maintain organ function. On the macro-level, treating the population involves public health measures, preventative vaccinations, and long-term lifestyle education to strengthen collective immunity against common threats.
One interesting point arises when comparing the speed of response required for different diseases. For rapidly progressing bacterial infections, treatment must often start immediately, sometimes empirically (before the exact pathogen is confirmed), because delays can be fatal. Conversely, boosting immunity through diet and exercise is a slow, cumulative process that yields benefits over months or years. This disparity forces clinicians and public health officials into a constant balancing act: applying immediate, powerful, but sometimes imperfect drugs now, while simultaneously investing in the slow-burn improvements that reduce the need for those drugs later. This necessity to address both immediate crisis and long-term resilience defines modern therapeutic strategy.
Furthermore, the economic and accessibility dimensions play a major role in effective treatment, even if they aren't direct medical procedures. A disease may be medically treatable—meaning a cure exists—but if the medication is unaffordable or unavailable in a particular region, the practical treatment success rate remains low. This is why organizations focus on making sure known, treatable conditions that cause high death tolls can actually reach the people who need them.
In summary, "How can diseases be treated?" has no single answer. It is an ongoing commitment involving cutting-edge pharmacology to neutralize specific threats, diligent supportive care to sustain the patient, robust public health initiatives to fortify the population's defenses, and ambitious global campaigns aimed at permanent elimination.
Related Questions
#Citations
Infectious Diseases: Types, Causes & Treatments - Cleveland Clinic
Infectious diseases - Diagnosis & treatment - Mayo Clinic
Prevention and Treatment - What You Need to Know About ... - NCBI
7 tips to fight disease and strengthen immunity
Healthy Habits: Enhancing Immunity - CDC
How to boost your immune system - Harvard Health
Eradication of infectious diseases - Wikipedia
Infectious Diseases - North Central Pa. - Treatment & Prevention
These 5 Diseases Are Treatable. They Kill Millions. | Partners In Health
Eradication of Diseases - Our World in Data