What is a certificate of need for hospitals?
A certificate of need (CON) acts as a state-mandated regulatory gatekeeper for healthcare providers looking to expand their services or facilities. [1] When a hospital, nursing home, or surgical center plans to introduce new medical equipment, build a new wing, or expand the scope of their clinical offerings, they often must secure this formal approval before proceeding. [2] The fundamental goal of these programs is to manage the growth of medical resources within a specific geographic area, ensuring that supply aligns with actual community demand. [5]
While the concept sounds straightforward, the execution varies significantly across the United States. In some jurisdictions, the process involves rigorous public hearings and data-driven analysis to prove that a new service is necessary for the population. [6] In others, the requirements are more streamlined, or in some cases, these laws have been repealed entirely, reflecting a shift in how different states view market competition in medicine. [3][7]
# Regulatory Purpose

The primary motivation behind these programs is the belief that healthcare does not function like a typical free market. [5] In most industries, if a business over-invests in capacity, it fails, and the market corrects itself. In healthcare, proponents argue that excessive investment in facilities and high-end technology can lead to increased costs for everyone. [1]
If two competing hospitals in the same small town both purchase expensive, high-tech imaging equipment, neither machine may be utilized to its full capacity. [1] To cover the fixed costs of these machines, both hospitals might raise prices for procedures to compensate for lower patient volumes. [9] By requiring a certificate of need, state regulators attempt to prevent this duplication of services. They require providers to demonstrate that the community genuinely needs the additional capacity, effectively putting a check on uncontrolled capital expenditures. [5]
Furthermore, these programs are often intended to protect access for vulnerable populations. By preventing providers from "cherry-picking" only the most profitable patients or locations, regulators hope to maintain a balance of care across an entire region. [10] The argument is that without such oversight, resources would naturally cluster in wealthy areas, leaving rural or underserved urban centers without adequate coverage. [5]
# State Variations
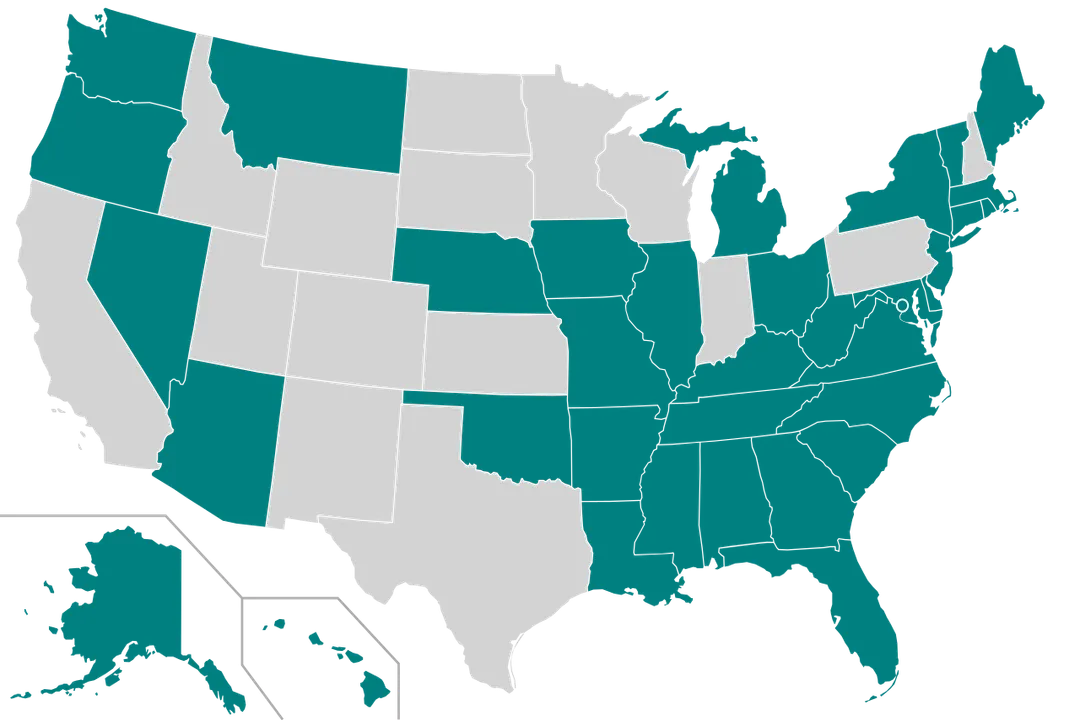
There is no single federal law governing these permits. Instead, the landscape is a patchwork of state-specific legislation. [3] According to the National Academy for State Health Policy, the requirements for these permits differ wildly from one border to the next. [7] Some states maintain highly active programs that review everything from the addition of a single hospital bed to the acquisition of specific diagnostic imaging tools. [2] Others have dismantled their programs, arguing that they create artificial monopolies and stifle innovation. [3]
States often categorize projects into different tiers. A minor equipment upgrade might undergo an expedited administrative review, while a project involving the construction of a new hospital or a major facility relocation requires a full, formal application process. [6] Tracking this requires checking individual state health department resources, as a list of regulated items in New York will not match the list in a state like Florida or Texas. [7]
# The Process
Securing a permit is rarely a quick task. It is a multi-step administrative procedure that requires substantial documentation and preparation. [6]
- Letter of Intent: The provider typically begins by submitting a formal notice to the state health department, outlining the proposed project, the projected costs, and the anticipated impact on the community. [6]
- Completeness Review: State regulators review the initial documents to ensure all required financial data, patient projections, and architectural plans are included.
- Public Comment: In many jurisdictions, the process includes a period for public input. Competitors often use this stage to challenge the proposed project, arguing that their existing facilities are already sufficient to meet the local demand. [4]
- Administrative Hearing: For major projects, a hearing may be held where the provider must testify and defend their data before a regulatory board or administrative law judge. [6]
- Decision: The state health department issues a final determination—either approving the certificate, denying it, or approving it with specific conditions, such as requirements to serve a certain percentage of Medicaid patients. [2]
This process can take anywhere from several months to over a year, depending on the complexity of the project and the level of opposition from competitors. [4]
# Market Impact
The economic impact of these laws remains a subject of intense debate. Critics, including many free-market economists and advocacy groups, argue that these programs serve as protectionist barriers. [4] They contend that established hospitals use the process to block potential competitors—such as outpatient surgical centers or specialized diagnostic clinics—from entering the market. [8]
By keeping competitors out, incumbent hospitals maintain their market share and are not pressured to lower prices or improve service quality. [4] This can result in limited patient choice. For example, a patient requiring an elective procedure might be forced to use a high-cost hospital outpatient department rather than a lower-cost, independent surgical center, simply because the state prevented the independent center from opening. [8]
Proponents of the programs, however, maintain that they are essential for cost control. [1] Without these barriers, they suggest that providers would engage in a "medical arms race," aggressively investing in unnecessary equipment to attract patients, which would drive up insurance premiums and overall healthcare spending. [5]
# Comparison Analysis
Understanding the tension between these two viewpoints helps clarify why these laws persist in some states but have disappeared in others.
| Feature | Pro-Regulation Perspective | Anti-Regulation Perspective |
|---|---|---|
| Market Impact | Prevents wasteful duplication of services | Creates barriers to entry for new competitors |
| Cost Control | Prevents unnecessary capital spending | Increases prices by reducing competition |
| Access | Protects services in underserved areas | Restricts access to modern facilities and technology |
| Quality | Keeps patient volume high at specialized centers | Stifles innovation and limits patient choices |
This comparison highlights that the impact is not universal. It often depends on the specific regulatory culture of the state. In a state with a well-managed program, the focus might be on ensuring rural access. In a state with heavy political influence, the program might indeed function more as a tool for incumbent facilities to preserve their market share. [4][5]
# Clinical Consequences
The impact on specific medical fields, such as oncology, is particularly distinct. [10] Cancer care requires high-cost technology and specialized infrastructure. When regulatory programs limit the ability of independent oncology practices to open infusion centers or acquire advanced diagnostic equipment, patients may have fewer options. [10]
Research in certain oncology sectors suggests that where these permits are required, patients might face longer wait times or be forced to travel further for routine treatments. [10] While the intention is to maintain quality by centralizing complex care, the unintended consequence can be a significant burden on patients who are already dealing with a difficult diagnosis. [10]
# Planning Checklist
For healthcare administrators or entrepreneurs considering a new project, navigating this landscape requires caution. Failing to recognize the need for a permit can lead to expensive legal delays or the total cancellation of a project after funds have already been committed.
If you are planning a healthcare venture, consider these preliminary steps:
- Audit Local Regulations: Do not assume your state’s laws are the same as the national average. Verify the current statute through the state’s Department of Health website. [2][6]
- Identify Triggers: Look for "thresholds" in the state law. For instance, does the law apply to any capital expenditure over $1 million? Does it apply to the acquisition of an MRI machine, regardless of cost?[2]
- Assess Competitor Risk: Anticipate that existing local facilities may oppose your application. Gather data early to prove that the community is currently underserved and that your project will fill a genuine gap, rather than just competing for existing patient volumes. [4][6]
- Engage Legal Counsel: Because these processes are quasi-judicial, having representation that understands the specific administrative law of that state is often a necessity, not an option. [6]
# Future Outlook
The trend in recent years has seen a gradual move toward scaling back these programs. [3] As the healthcare industry shifts toward value-based care and outpatient services, many states are reevaluating whether the traditional "gatekeeper" model makes sense in the modern era. [3]
Some states have begun to exempt certain types of services from the process, particularly outpatient procedures and diagnostic testing, while keeping oversight for major inpatient facility construction. [7] This "partial" approach attempts to find a middle ground, allowing for more competition in lower-cost settings while maintaining control over the largest, most expensive hospital investments. [8]
Ultimately, the certificate of need remains a controversial and complex element of the American healthcare landscape. For patients, it represents a layer of government oversight that can either protect them from unnecessary medical inflation or prevent them from accessing more convenient, lower-cost care. For providers, it is a significant regulatory hurdle that defines where and how they can serve their communities. As states continue to adjust their policies, the role of these permits will likely remain in flux, reflecting the ongoing struggle to balance market competition with the containment of rising healthcare costs. [3][5]
Related Questions
#Citations
Understanding Certificate of Need (CON) in Healthcare
Certificate of Need (CON)
Brief Certificate of Need State Laws
Certificate of Need (CON) Frequently Asked Questions
Certificate of need
Health Facilities | Certificate of Need and Facility Licensing
50-State Scan of State Certificate-of-Need Programs
Certificate of Need Laws Explained
Certificate of Need (CON)
Understanding “Certificate of Need Laws” and How They Limit ...


